Gynecologic cancers are those that originate in the female reproductive organs. They include ovarian cancer, cervical cancer, uterine (endometrial) cancer, vaginal cancer and vulvar cancer. Identification of risk factors and early detection are crucial to improve survival rates and treatment outcomes.
Gynecologic cancers represent a diverse group of malignancies affecting women. Each type of gynecologic cancer has its own set of risk factors and screening methods, but all share the importance of early identification for successful treatment. Understanding these factors and the screening options available can save lives and significantly improve patients' quality of life.
Risk factors for gynecologic cancers
Gynecologic cancers can be influenced by a variety of risk factors. Understanding these factors is essential to identifying women at increased risk and taking appropriate preventive measures. Risk factors may vary depending on the specific type of gynecologic cancer, but there are some common ones that affect overall gynecologic health. Below, we will explore in detail the main risk factors associated with each type of gynecologic cancer, helping women become more informed and proactive in their healthcare.
Ovarian cancer
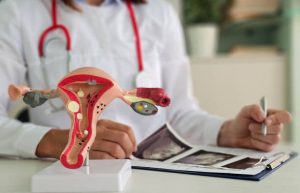
Ovarian cancer is a form of cancer that originates in the ovaries, the female reproductive glands responsible for producing eggs as well as hormones such as estrogen and progesterone. There are several types of ovarian cancer, the most common being epithelial carcinoma, which develops in the layer of cells covering the outside of the ovaries. Other types include germ cell tumors and stromal tumors, which are less common but also originate in the ovaries.
- Age: The risk increases with age, especially after 50 years of age.
- Family history: Having close relatives with ovarian or breast cancer.
- Genetic mutations: Mutations in the BRCA1 and BRCA2 genes.
- Reproductive history: Not having had children or having had children after the age of 35.
- Hormone therapy: Use of hormone therapy after menopause.
Cervical cancer
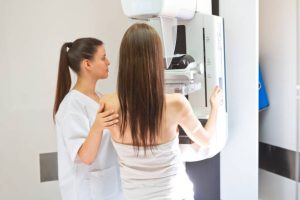
Cervical cancer is a type of cancer that develops in the cells of the cervix, the lower part of the uterus that connects to the vagina. It is commonly caused by the human papillomavirus (HPV) and can be prevented by vaccination and detected in its early stages through Pap smears and HPV testing.
- Infección por VPH: El virus del papiloma humano es el principal factor de riesgo.
- Smoking: Smoking increases the risk of cervical cancer.
- Weakened immune system: Due to HIV/AIDS or other conditions.
- Sexual history: Having multiple sexual partners or sexual intercourse at a young age.
Cancer of the uterus (endometrium)
Uterine cancer, also known as endometrial cancer, is a type of cancer that originates in the inner lining of the uterus, called the endometrium. It is the most common type of uterine cancer and usually manifests itself through symptoms such as abnormal vaginal bleeding. Endometrial cancer is more common in postmenopausal women and is associated with risk factors such as obesity, hormone therapy and certain medical conditions such as polycystic ovary syndrome (PCOS).
- Age: Higher incidence in postmenopausal women.
- Hormone therapy: Prolonged use of estrogen without progesterone.
- Obesity: Excess weight increases estrogen levels.
- Polycystic ovary syndrome (PCOS): Affects hormone levels.
- Diabetes: It is associated with an increased risk.
Vaginal and vulvar cancer
Vaginal cancer
Vaginal cancer is a rare type of cancer that forms in the tissues of the vagina, the muscular canal that connects the uterus to the outside of the body. This cancer can develop in the cells that line the surface of the vagina and, in its early stages, often has no symptoms, although it may manifest itself with abnormal vaginal bleeding, pain during intercourse or the appearance of a lump in the vagina.
Vulvar cancer
Vulvar cancer originates in the vulva, the external part of the female reproductive system, which includes the labia, clitoris and vaginal opening. This type of cancer usually affects older women and may present with symptoms such as persistent itching, pain, changes in the color or thickness of the vulvar skin, and the appearance of lumps or sores.
- Advanced age: More common in women over 60 years of age.
- HPV infection: Main risk factor.
- History of dysplasia: Precancerous changes in vaginal or vulvar cells.
- Weakened immune system: Increases the risk of infections and cancer.
Early detection and appropriate treatment are crucial to improve outcomes in both cases.

Early detection of gynecologic cancers
Early detection of gynecologic cancers significantly improves the chances of successful treatment and reduces mortality. Screening programs and regular visits to the gynecologist are essential to identify precancerous changes and early stage cancers. Education about risk factors and symptoms is also crucial for women to seek timely medical care.
Ovarian cancer:
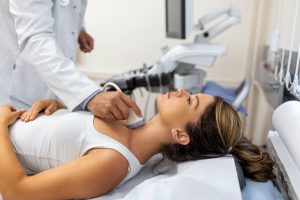
- Transvaginal ultrasound (TVUS): Uses sound waves to create images of the ovaries.
- CA-125 test: Measures the level of CA-125 in the blood, which may be elevated in cases of ovarian cancer.
- Genetic risk assessment: Testing for BRCA1 and BRCA2 mutations.
Cervical cancer:
- Papanicolaou (Pap) test: Detects abnormal cells in the cervix that can develop into cancer.
- HPV test: Detects the presence of the human papillomavirus, which can cause cervical cancer.
Cancer of the uterus (endometrium):
- Endometrial biopsy: Takes a sample of tissue from the lining of the uterus to look for cancer cells.
- Transvaginal ultrasound: Evaluates the thickness of the endometrium.
Vaginal and vulvar cancer:
- Pelvic examination: Visual and manual evaluation of the vagina and vulva for abnormalities.
- Biopsy: Removal of a tissue sample for analysis if suspicious areas are found.
Understanding risk factors and the importance of early detection is critical in the fight against gynecologic cancers. At Panama Cancer Clinic, we are committed to providing education, state-of-the-art screening tools and treatment to help women prevent and fight these cancers. If you have questions or need more information about our screening and treatment options, please do not hesitate to contact us.