Colonoscopy
Colon and rectal cancer is the third most frequent type of cancer in the world. Colonoscopy is a medical procedure that saves thousands of lives every year; its main objective is to explore the large intestine and colon in search of any abnormal changes (inflammation or irritation in the tissues, polyps or neoplasms).
What is colonoscopy?
Colon and rectal cancer is the third most frequent type of cancer in the world. Colonoscopy is a medical procedure that saves thousands of lives every year; its main objective is to explore the large intestine and the walls of the colon in search of any abnormal changes (inflammation or irritation in the tissues, polyps or neoplasms).
How is colonoscopy performed?
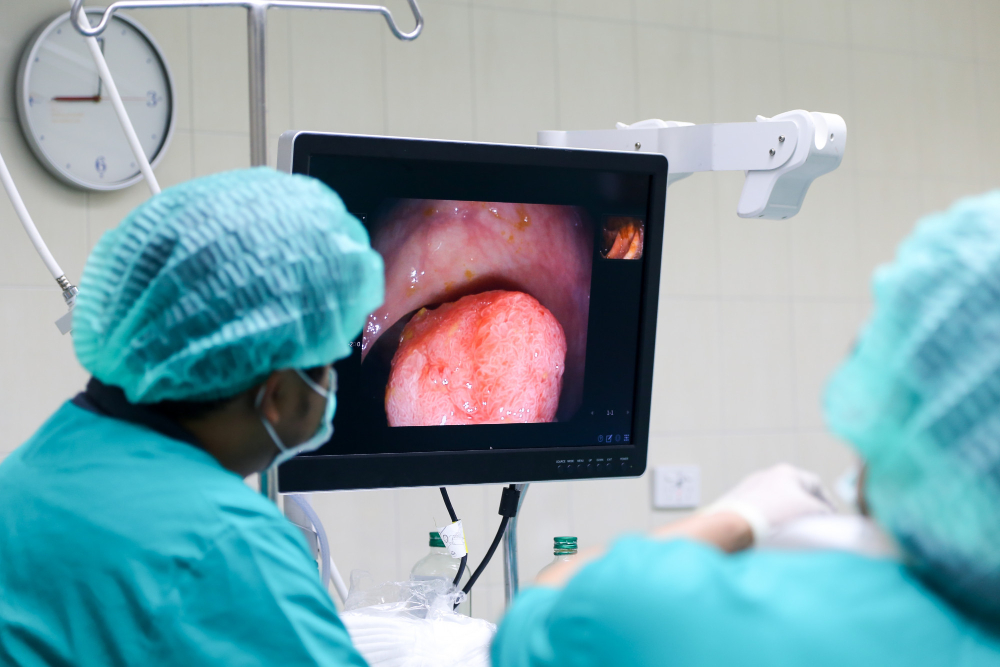
Colonoscopy uses a special instrument called a colonoscope, which consists of a flexible, elongated probe with a camera attached to its tip through which the images obtained are transmitted live to a monitor.
The procedure begins by administering sedatives and painkillers intravenously to the patient to avoid discomfort or discomfort during the examination. Subsequently, the physician slowly introduces the colonoscope through the anus until the entire surface of the rectum and colon is covered internally.
Through the same colonoscope tube, additional instruments may be introduced for the purpose of taking a biopsy (tissue samples) or performing the removal of polyps or other suspicious masses. Colonoscopy is a short-term examination that usually takes between 30 minutes and 1 hour in total.
The effects of the sedative usually wear off within an hour after the procedure is completed; it is essential that the patient be assisted by a family member or friend to leave the clinic and get home safely.
When is colonoscopy necessary?
Your doctor may recommend a colonoscopy for the following reasons:
The patient presents with abdominal pain, weight loss or alterations in bowel movements.
Polyps have been found in other previous examinations.
Iron deficiency anemia has appeared for no apparent reason.
The stool is bloody or has a dark color that is not normal.
To follow up the diagnosis of a previous disease (cancer, polyps, etc.).
To thoroughly evaluate inflammatory bowel disease, such as Crohn's disease or ulcerative colitis.
How to prepare for a colonoscopy?
Unlike other types of tests, colonoscopy does require meticulous preparation beforehand. In this regard, the patient must clean the walls of the colon and make sure to remove any debris inside the intestine, in order to prevent it from interfering with the quality of the images taken during the examination.
Likewise, the patient should discuss with the specialist his or her medical history, allergies and frequently used medications, since some of them may be counterproductive.
What you should avoid eating
As part of the preparation of the colon and bowel prior to a colonoscopy, it is generally recommended that solid foods and certain types of foods be avoided to ensure adequate bowel cleansing.
These are the foods to avoid before a colonoscopy:
- Foods rich in fiber: Foods that are rich in fiber such as raw fruits and vegetables, whole grains, nuts and seeds increase stool bulk and hinder adequate visualization during colonoscopy.
- Dairy products: Some dairy products, such as whole milk and fatty cheeses, are difficult to digest and may leave residues in the colon.
- Fatty or fried foods: Fried foods, fast foods and fatty foods cause slower digestion and thus leave undesirable residues on the walls of the colon.
- Red meat: Red meat is very difficult to digest, so it tends to increase waste production in the colon.
- Alcoholic beverages: Alcohol consumption affects the colon cleansing process and interferes with the medications used during colonoscopy.
Is colonoscopy covered by insurance?
The limits of insurance coverage will depend on the insurance company and the plan contracted. However, we can mention that there are many insurance companies that include colonoscopy in their policies, as it is an essential screening test for people with a high risk of colon cancer.
To verify whether or not your insurance covers colonoscopy, we invite you to contact your insurance advisor.
Gardasil® 9
It could be said that Gardasil® 9 is an improved version of Gardasil®. This vaccine, in addition to preventing people from contracting the 2 genotypes most at risk for cervical cancer, also acts against oncogenic types 6 and 11 (which cause 90% of genital warts) and 5 other genotypes responsible for cancer.
Results obtained from the colonoscopy

After interpreting the images obtained during the colonoscopy, the specialist will explain the results to the patient. It should be noted that if the imaging does not show conclusive results because of poor visualization due to residual stool in the bowel, the physician may advise repeating the examination within the next few days.
Negative colonoscopy
A negative colonoscopy indicates that the physician has found no evidence of abnormalities in the colon. It is likely that the specialist will recommend another colonoscopy in 7 to 10 years; everything will depend on how low the patient's risk factors for colon cancer are, previous medical history or predisposition to genetic syndromes.
Positive colonoscopy
When a colonoscopy yields positive results, it is because during the test the physician noticed abnormal tissues or performed the removal of relevant polyps in some section of the large intestine. About 90% of polyps are non-neoplastic; however, a small percentage may be precancerous.
The polyps extracted in a colonoscopy are sent to the laboratory for evaluation, determining with certainty the nature of the polyps (cancerous, non-cancerous or precancerous).
If multiple polyps of different sizes were found during the examination, it is very likely that the physician will advise active surveillance of these lesions in order to discover new polyps at an early stage.
Risk Factors
Risk factors for colonoscopy refer to circumstances that may increase the likelihood that a person will experience complications or adverse effects during or after the procedure. Some common risk factors are:
- Advanced age: As a person ages, there may be an increased risk of complications during a colonoscopy.
- Pre-existing health conditions: People with heart disease, lung disease or diabetes, are at a higher risk of complications during the procedure.
- Medications: Certain medications, such as: anticoagulants or diabetes drugs, often increase the risk of bleeding or complications.
- History of abdominal surgery: People who have had previous abdominal surgery are more prone to complications during colonoscopy due to the presence of adhesions or scarring in the area.
- Obesity: Obesity can make the colonoscopy procedure more difficult and increase the risk of complications due to poor visualization of the area.
Symptoms and Conditions Associated with Colonoscopy
During and after a colonoscopy, certain symptoms and conditions associated with the procedure may occur. Among them we can mention:
- Abdominal discomfort: It is common to experience some degree of abdominal discomfort after a colonoscopy. This may manifest as bloating, gas or cramping. These symptoms usually disappear within a short time.
- Rectal bleeding: After a colonoscopy, you may notice slight rectal bleeding; this is normal and is usually caused by the removal of polyps or biopsies. Bleeding should be minimal and stop within a short time, but if bleeding is heavy or persistent, the physician should be informed.
- Changes in bowel habits: Some people may experience temporary changes in their bowel habits after a colonoscopy. This may include diarrhea or mild constipation for a short time.
- Allergic reactions: In very rare cases, a person may experience allergic reactions to the medications used during colonoscopy. If difficulty breathing, swelling in the face or hives are experienced, it is necessary to seek medical attention immediately.
Frequently Asked Questions - Colonoscopy
The colonoscopy will not be painful for the patient as long as he/she remains sedated; however, after the procedure there may be slight discomfort, slight rectal bleeding and a (temporary) swelling sensation in the abdominal area as a result of the air pumping used during the colonoscopy.
The frequency of colonoscopy will be more or less depending on the different individual risk factors. People with direct relatives who have suffered colorectal cancer are more prone to develop the disease; therefore, they should undergo the test before their 45th birthday.
Patients who have had polyps removed at previous colonoscopies may need to be re-screened every 3 years. Colon or rectal cancer survivors also warrant regular screening as recommended by their treating physician.
People who suffer from ulcerative colitis or Crohn's disease should undergo colonoscopy in periods of 1 to 2 years because they have a high risk of colorectal cancer.
In order to minimize the risks during pregnancy, it is most prudent that the colonoscopy be postponed until the mother gives birth. In cases of extreme urgency, the specialist and the patient should weigh the pros and cons of the procedure before making a decision.
Although colonoscopy is generally a safe test, there will always be a percentage risk that something will not happen as planned. Possible complications of a colonoscopy include:
- Allergic reaction to the sedative administered.
- Rectal bleeding resulting from polyp removal or biopsy.
- Abdominal pain.
- Cramps that persist for a few days.
- Perforation of the intestinal wall.
- Infections (unusual).