Cervical Cancer
It is a disease caused by the presence of malignant cells in the tissue lining the uterine cervix. The human papillomavirus (HPV) is considered the main triggering factor in the appearance of cervical cancer.
Integral medical support in your oncologic process
At Panama Cancer Clinic we provide a complete medical approach, guiding our patients with commitment and dedication at every stage. We establish personalized care plans and we do not stop until we help them successfully overcome their pathologies.

Cervical cancer is included among the 5 types of cancer with the most diagnoses in the female population.

Signs of cervical cancer may go unnoticed in its early stage; however, a Pap smear can detect any abnormalities in this area early.
Planning and Organization
Knowing what stage (stage) your cervical cancer is in will help us determine precisely what treatment is most effective for you.

General Welfare
In order to achieve the best possible results, each of our patients is evaluated by professionals in the area of nutrition and oncological psychology, giving a comprehensive approach to their medical plan.
The Specialist
The joint work of our oncology specialists allows us to obtain a broader perspective of the treatment to be implemented; following the execution of the plan to achieve satisfactory results.
What is cervical cancer?
Cervical cancer is a disease that comes from the uncontrollable growth of the glandular or squamous cells that line the lower part of the uterus. Internally, the cervix is made up of the endocervix (area lined by glandular cells) and the exocervix (area lined by squamous cells).
Types of cervical cancer
In cervical cancer, 2 types predominate, which we will detail below:
Squamous cell carcinoma:
About 90% of cervical cancers are of this type; being the squamous cells of the exocervix that develop in favor of cancer.
Cervical adenocarcinoma:
A large part of the remaining percentage of cervical cancer corresponds to the adenocarcinoma family; it emerges from the glandular cells responsible for the production of mucus within the endocervix.
There is a third very rare type of cervical cancer called squamous adenocarcinoma or mixed carcinoma; which simultaneously presents malignant characteristics in both squamous cells and glandular cells.
Symptoms of cervical cancer
Initially, the signs of cervical precancer are usually virtually unnoticeable; however, as the cancer progresses, so do its signs. When the disease reaches a point where it has increased considerably in size or has spread to other parts, the patient may show signs more frequently:
Pelvic pain.
Vaginal bleeding after intercourse.
Menstrual bleeding in menopausal women.
Irregular menstrual periods.
Abnormal vaginal discharge or visible changes in vaginal discharge.
Fatigue.
Nausea.
Weight loss.
Contact us at
Schedule an appointment
Request a consultation
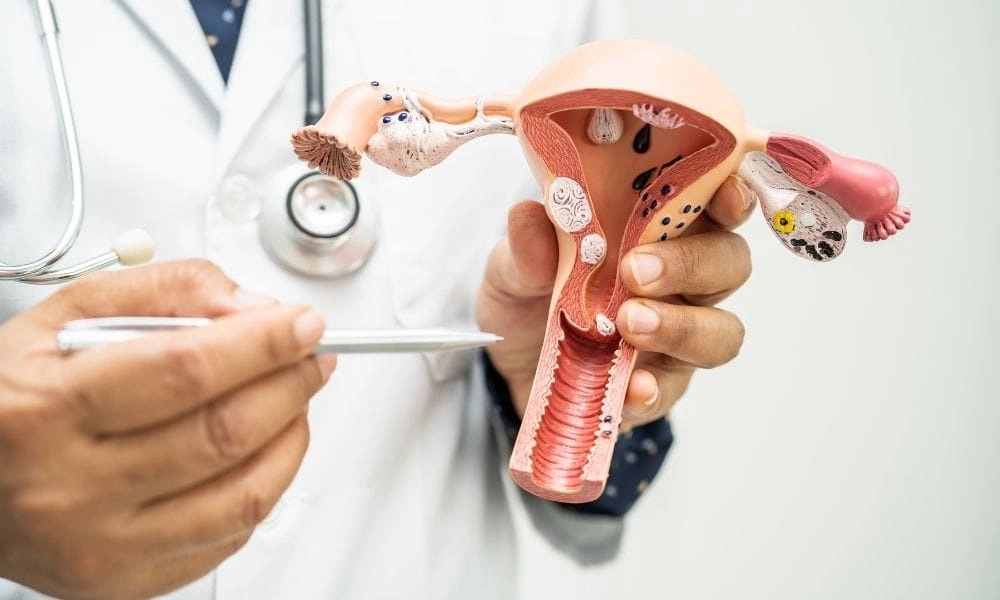

Risk Factors
The presence of one or more risk factors can increase the chances of developing cervical cancer; however, this is not a determining factor. There are many women who have some of them, and still do not have cancer.
Risk factors associated with cervical cancer are:
Sexual history, especially when HPV (primary), HIV or chlamydia infections are present.
Smoking.
Compromised immune system; either by suffering from autoimmune diseases or by having an organ transplant.
Prolonged use of contraceptives.
Have had more than 3 full-term pregnancies.
Diet low in fruits, vegetables and greens.
Family history of cervical cancer.
Screening tests
How to detect cervical cancer?
It is advisable to start cervical cancer screening at an early age (around 25 years of age).
To do this, the person can be tested for human papillomavirus (HPV) every 5 years, or alternatively, Pap smears every 3 years.
The dissemination of information on this topic and the worldwide increase in the use of the aforementioned screening tests have helped to considerably decrease the mortality rate from cervical cancer.
Prevention
How to prevent cervical cancer?
Maintain condom-protected sex, have routine screening tests, and get the human papillomavirus vaccine.
These are some of the smartest preventive actions you can take against cervical cancer. The progression of cervical cancer is not as aggressive compared to other types of cancers. So, catching precancer before it becomes invasive and treating it early can mean a big advantage in the recovery process.
Cervical cancer treatments
Depending on the stage of your cancer, your doctor can suggest the most appropriate treatment options. In this treatment plan, factors such as age, current health status and the patient's particular preferences are taken into consideration.
The most common ways to treat cervical cancer are:
Simple hysterectomy surgery:
In this procedure, the oncological surgeon is in charge of removing the uterus, but not the structures close to it, for example: ovaries, parametrium, ligaments or lymph nodes.
Radical hysterectomy surgery:
Operation to remove the uterus, parametrium and uterosacral ligaments.
Radiotherapy:
In this procedure, high-impact X-rays are used to eliminate malignant cancer cells.
Chemotherapy:
In chemo, oral or intravenous drugs are administered, which travel through the bloodstream until they find the exact point where the cancer resides in order to attack it.
Targeted drug therapy:
This method is totally different from chemotherapy, although both are aimed at eliminating the cancer. In targeted therapy, the proteins that feed the growth of the disease are directly attacked; in this way, the "life" of the cancer can be destroyed or stopped.
Immunotherapy:
In immunotherapy, the oncologist provides drugs to strengthen and reinforce the patient's immune system, with the intention that the body itself learns to recognize and eliminate the malignant cells that inhabit it.


Complications in Cervical Cancer Treatment
Among the possible setbacks that patients with cervical cancer may face, we have:
Risk that the cancer will recur some time after recovery.
Suffer sequelae that prevent proper sexual, urinary or bowel function.
Additionally, each method of treatment or procedure applied brings with it its own consequences, for example: Removal of the uterus by surgery will inevitably cause infertility in the patient. On the other hand, radiotherapy and chemotherapy can cause kidney problems.



