From the appearance of genital warts to the formation of lesions that can evolve into cancer in the cervix, vagina and vulva, the Human Papilloma Virus can have various manifestations. In order to prevent, early detection through tests such as the Pap smear is fundamental.
The Human Papilloma Virus has more than 240 genotypes, of which 15 are linked to various types of cancer, such as cervical, vaginal, vulvar, anal and oropharyngeal (which includes the back of the tongue, palate, throat and tonsils). Among the most important genotypes are 16 and 18, which are responsible for 70% of cervical cancers.
Transmission occurs primarily through sexual contact, including vaginal, anal and oral intercourse. It is important to note that HPV is the most common sexually transmitted infection worldwide, so it is estimated that more than 80% of sexually active women and men will at some point contract Human Papillomavirus (HPV). However, not all HPV infections will progress to cancer. Approximately 90% of these infections are temporary and people clear them through their own natural immunity or defenses.
The effects of papillomavirus in women are divided into benign and malignant lesions. Between infection and cancer, premalignant lesions occur, which have a high risk of progressing to cancer. As for the period between HPV infection and the manifestation of cancerous lesions on the cervix, the duration will depend on the individual's immune response. In general terms, it is estimated that at least 10 years must elapse between infection and the appearance of invasive cancer, although pre-invasive lesions may appear two years after infection.
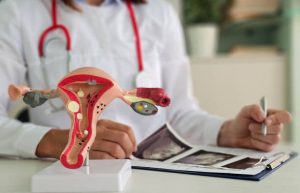
The Connection Between HPV and Cervical Cancer
Cervical cancer is the most important consequence of HPV. According to WHO, it is the fourth leading cause of cancer in women worldwide, with an estimated incidence of 604,000 new cases and 342,000 deaths by 2020. These statistics underscore the importance of understanding the connection between HPV and cervical cancer. The good news is that we can prevent its development, and detect it even before it becomes cancer, and treat it to prevent the development of this disease. How can we do this?

HPV vaccination:
Currently, there are WHO-endorsed vaccines that provide protection against Human Papillomavirus (HPV) types 16 and 18, which are responsible for at least 70% of cervical cancers. The nonavalent vaccine also protects against five other oncogenic HPV types, which cause approximately another 20% of cervical cancer cases.
Importantly, these vaccines are most effective when administered prior to HPV exposure. Therefore, vaccination is recommended for girls aged 9 to 14 years, before most become sexually active.
"It is crucial to understand that vaccination does not replace screening for premalignant lesions (LIEAG)."
Papanicolaou (Pap) smear tests
These tests are critical for the early detection of cellular changes in the cervix caused by HPV. Early detection through the Pap test is crucial to prevent the development of cervical cancer.
HPV Test
This test checks for the presence of high-risk viruses in the cervix and is a valuable tool for early detection. Its inclusion in screening programs has significantly improved the identification of women at risk.
Prevention plays a key role in HPV management and cervical cancer risk reduction. Some crucial strategies, other than vaccination, are highlighted here:
-
Safe sexual practices:
Condom use can reduce the risk of HPV transmission, although it does not completely eliminate it. Education on safe sex practices is essential.
-
Monitoring and medical care:
Women should undergo regular gynecological examinations and follow the recommendations of health professionals for monitoring and treatment. Early detection and appropriate treatment are crucial.
HPV, being the most common sexually transmitted infection, has significant implications for women's health, especially in relation to cervical cancer. Prevention, early detection and appropriate treatment are fundamental pillars in the management of this infection. Ultimately, awareness, education and access to health services play a crucial role in the fight against HPV and its consequences, highlighting the importance of a comprehensive approach to address this public health issue.